AI document processing for insurance claims handling
Claims teams don’t need more paperwork – they need faster decisions. Affinda automates claims document processing with AI, turning claim forms, invoices and evidence into structured data you can use.Describe your exact workflow
Tell the agent what needs to happen in your insurance claims handling process and where the results should go.Automate claims handling workflows
Stop wasting time on manual processing
Manual handling slows down claims decisions and increases operating costs. We help you automate claims document processing so your team spends less time keying data and more time assessing coverage, liability and outcomes.Accelerate claims approval timelines
Delays often happen when claim documents need to be reviewed, checked and re-entered into a claims system. We enable faster straight-through processing by extracting key fields and applying validation rules, so low-risk claims move through faster, and complex claims reach the right handler sooner.Improve accuracy, eliminate errors
Manual data entry and document interpretation lead to errors, missed details and inconsistent outcomes. Our AI platform delivers high-accuracy extraction that adapts continuously to every document and human interaction.Scale claims volume without stretching teams
As claim volumes rise, manual workflows become a bottleneck. We help claims teams process more claim documents without additional headcount, improving throughput during peaks, catastrophes and seasonal surges.Stay compliant and secure
Claims teams need traceability across every decision. We maintain a clear record of every document processed, where every extracted field came from and every rule that’s applied, supporting compliance, dispute resolution and audit readiness.Extract any information from any document, fast
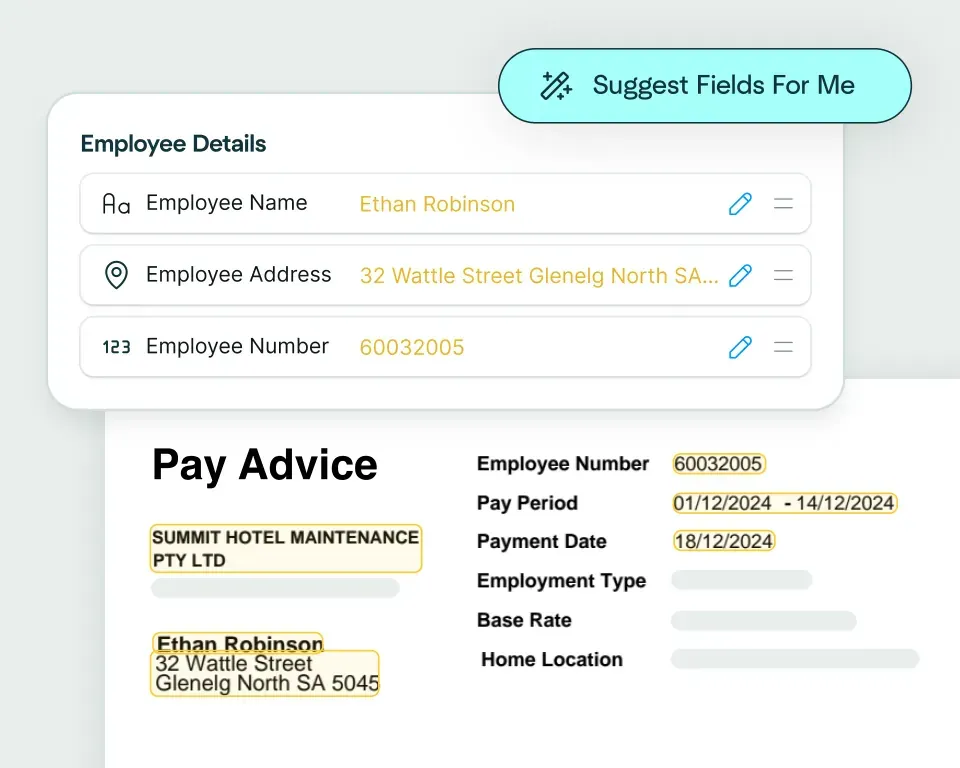
Create models in seconds
Upload a claims document and the Affinda Platform will predict the fields you need – like claimant details, policy number, incident date, totals and line items – so you can automate claims document processing in just a few clicks.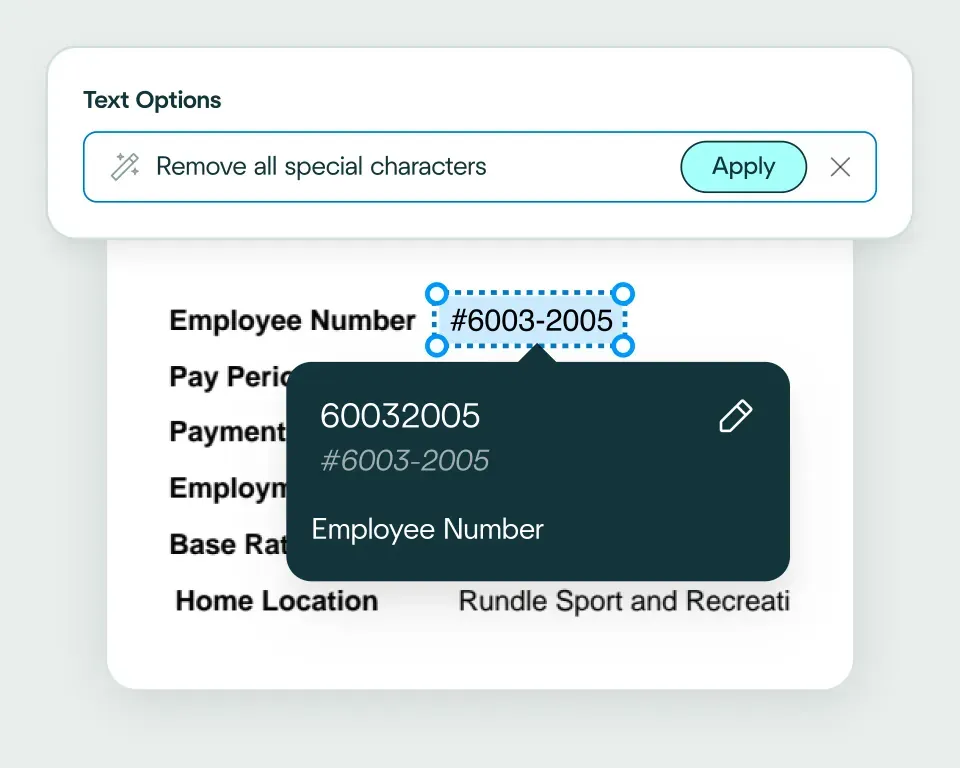
Validate and transform data
The platform checks extracted claims data against your business rules and transforms it into a format your claims management system expects. That way, it’s ready for workflows like coverage checks, reserving, routing and settlement.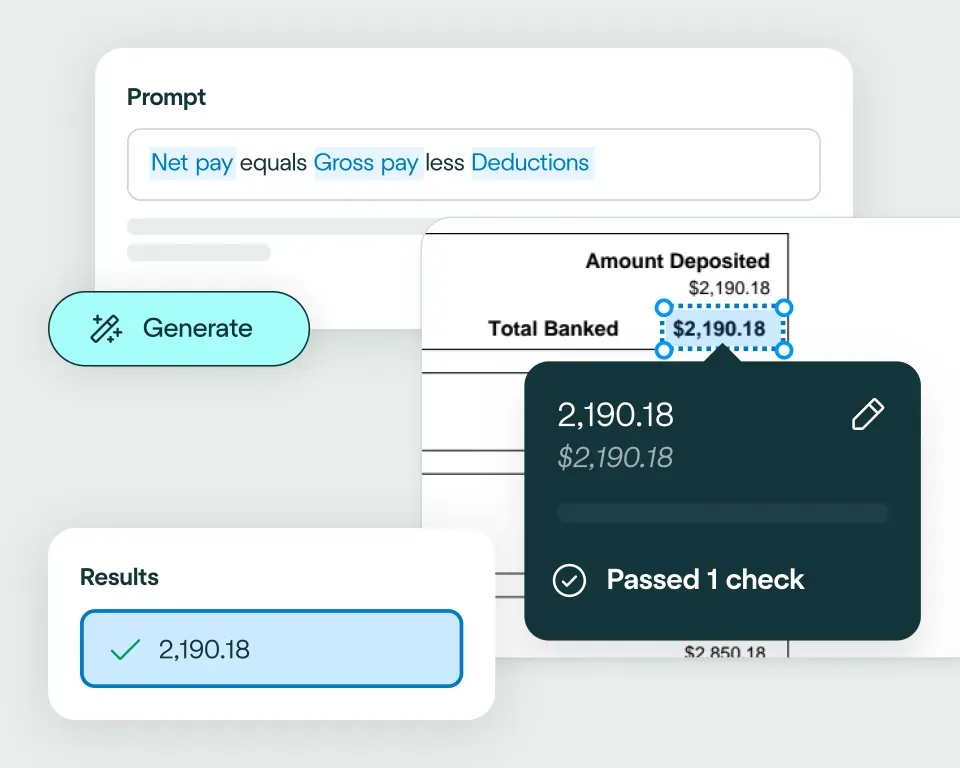
Apply your business logic
Use natural language to write validation rules that match your claims workflows, for example: flag missing fields; check policy numbers match correct formats; validate that document dates are within ranges; check financial consistency, such as line items summing correctly to totals.Pathway 1: Use the Agent
Create integrations fast, even if you’re not a developer. Choose from 2800+ business systems and describe how you want your claims document processing workflow to connect, using natural language. The Agent will generate the code to make it happen.Pathway 2: Write your own code
Easily connect Affinda Platform to your claims stack using our client libraries and APIs. Automatically generate type-safe Pydantic models or TypeScript interfaces tailored to your claims documents, so extracted fields map cleanly into your workflows.Claims intake
Digitize claim forms and validate against required fields and your reference data, so only complete, accurate claims enter your system.Evidence review
Extract key details from tax returns, medical records, financial statements, invoices and supporting documents, then check for consistency and flag anomalies.Fraud detection
Highlight inconsistencies across submitted documents and flag anomalies for review earlier in the claims process.Policy validation
Verify extracted claims data against your records, verifying policy numbers, claim limits and eligibility requirements, before claims proceed.Settlement support
Review settlement packs and supporting documentation before payout approval, reducing errors and improving auditability.Customer communication
Process correspondence and route it to the right claim handler, leading to faster responses, fewer delays and better claimant experience.No need to talk to sales. Get started now
With a free trial, discover how easy it is to extract any information from any document, fast.Sign up for free
No sales calls, no credit cards and no hidden features. Get all the power in your hands from day one.Upload documents
Drag and drop, email or upload via API. Affinda can handle any document, any file type and any layout with ease.See the magic
Watch as the platform predicts the information you want to extract, letting you build models in minutes, not months.Automating their document processes with AI
Combine the best of artificial and human intelligence

Frequently asked questions
What is intelligent document processing for claims processing?
Intelligent document processing (IDP) for claims processing uses AI to extract, validate, and structure data from claims documents – like claim assessments, invoices, medical reports, police reports and repair estimates.
How does AI help optimize claims handling workflows?
AI speeds up claims handling by removing manual steps across intake, evidence review and settlement. We extract key fields automatically, validate them against your rules and route exceptions to the right handler.
What types of claims documents can you process?
We process a wide range of claims documents, including:
What are best practices for automating claims intake documents?
Some best practices we recommend:
What does claims OCR mean – and is OCR enough on its own?
Claims OCR typically refers to using optical character recognition to convert claim documents into text. That’s useful, but OCR alone doesn’t understand context, identify the right fields, or validate information.
Can you automate CMS-1500 claim form OCR and extraction?
Yes. The CMS-1500 has consistent field labels, but real-world submissions still vary – different scans, handwriting, highlights and layout changes.
Do you support OCR red claim forms or scanned, low-quality claim documents?
We support difficult inputs, including low-resolution scans, skewed pages, noisy backgrounds and colored forms. If you’re dealing with “red” or heavily marked claim forms, we can still extract the key fields and route uncertain values for review.
Can your AI validate claims data against policies and business rules?
Yes – validation is where claims automation becomes truly useful. We can apply rules like:
How does automated document processing support fraud checks in claims?
Fraud indicators often appear across multiple documents – mismatched dates, inconsistent names, altered invoices or repeated patterns.
Can insurance companies use RAG to automate claim document analysis?
Yes. Many insurers use retrieval-augmented generation (RAG) to ask questions across a claim file – for example, “Does this claim include proof of ownership?” or “What is the total claimed amount across all invoices?”
Are you HIPAA-compliant for claims document automation?
Claims workflows often include sensitive personal information. We take security seriously and support enterprise-grade controls for handling confidential documents.
What kinds of claims can you support (health, travel, motor, pet, warranty)?
We support claims workflows across many lines, including:
Why is extraction alone not enough for claims document automation?
LLMs and AI models can extract data from claims documents with impressive accuracy. The harder challenge is knowing whether that data is correct, complete and safe to use in production. Affinda goes beyond extraction to validate outputs against your business rules, ground data back to source documents for verification, route exceptions for human review and maintain full audit trails.